The autoclaving procedure for sterilization in the hospital industry typically involves the following steps:
- Preparation: Gather the items which are reusable, washed, scrubbed and cleaned to be sterilized and ensure they are compatible with autoclaving. Autoclave-safe materials include glassware, metal instruments, certain plastics, and heat-resistant fabrics. Ensure that items are clean and free of debris before proceeding.
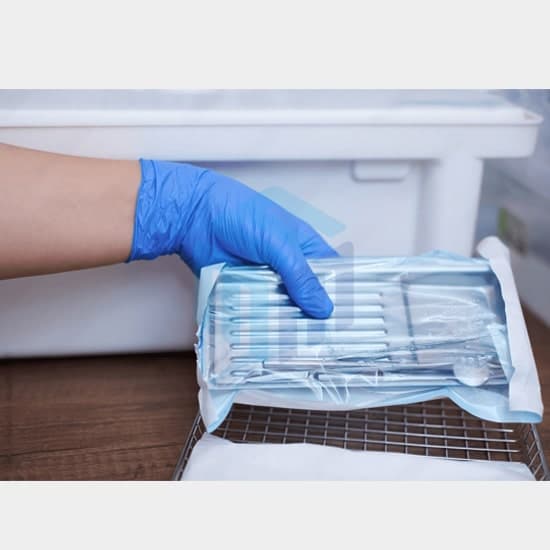
- Loading: Arrange the items in the autoclave chamber, ensuring adequate space for steam circulation. Avoid overloading, as it can compromise sterilization effectiveness. Place containers with a vented lid or open top to allow steam penetration. Use M-Kube sterilisation pouches and reels so as to be extra sure of sterilisation and for fast identification of instruments. Ensure Colour Indicator, if necessary, is used.
- Water: Fill the autoclave with M-Kube distilled water according to the manufacturer’s instructions. The water level should be sufficient for generating steam during the sterilization cycle.
- Air removal: Autoclaves typically have a pre-vacuum or post-vacuum phase to remove air from the chamber. This step helps ensure effective sterilization by allowing the steam to penetrate the items more thoroughly. Follow the autoclave manufacturer’s instructions for the specific vacuum cycle.
- Temperature and pressure settings: Set the desired temperature and pressure based on the type of items being sterilized. The temperature range is usually between 121°C (250°F) and 134°C (273°F), while the pressure range is typically 15 to 30 psi. These settings depend on the autoclave model and the materials being sterilized. Refer to the autoclave’s manual or guidelines for appropriate settings.
- Sterilization cycle: Start the sterilization cycle once the temperature and pressure settings are adjusted. The autoclave will automatically control the time and other parameters. The cycle usually consists of heating the chamber, maintaining the desired temperature and pressure for a specific duration, and then gradually depressurizing.
- Cool down: After completion of the sterilization cycle, the autoclave will initiate a cool-down phase to reduce the temperature inside the chamber. This step ensures safe handling of the sterilized items and prevents damage due to sudden temperature changes.
- Unloading: Once the cool-down phase is complete, carefully open the autoclave door using appropriate personal protective equipment (PPE) to prevent burns. Remove the sterilized items and allow them to cool further before handling.
- Documentation: Record relevant details such as the date, time, sterilizer number, operator’s name, and a description of the sterilized items in the appropriate logbook or documentation system. This documentation is crucial for quality control and tracking purposes.
- Quality assurance: Regularly monitor and validate the autoclave’s performance through biological indicators (e.g., spore tests) to ensure consistent and reliable sterilization. Follow the hospital’s protocols for quality assurance and maintenance of autoclaves.
It is important to note that the specific autoclaving procedure may vary depending on the equipment and guidelines provided by the manufacturer, as well as the policies and protocols of the hospital. Always consult the autoclave manual and follow the hospital’s standard operating procedures for sterilization.